-
Články
Top novinky
Reklama- Vzdělávání
- Časopisy
Top články
Nové číslo
- Témata
Top novinky
Reklama- Kongresy
- Videa
- Podcasty
Nové podcasty
Reklama- Kariéra
Doporučené pozice
Reklama- Praxe
Top novinky
ReklamaConservative and surgical treatment of fractures of articular process of mandible in adults
Authors: Jan Štembírek 1; Anna Ščerbová 1; Marta Litshmanová 2; Oldřich Res 1; Jiří Stránský 1
Authors place of work: Klinika ústní, čelistní a obličejové chirurgie, Fakultní nemocnice Ostrava 1; Katedra aplikované matematiky, Fakulta elektroinformatiky, Vysoká škola báňská Ostrava 2
Published in the journal: Úraz chir. 26., 2018, č.4
Summary
Surgical treatment of fractures of the articular process of mandible is one of the most complicated procedures in facial skeletal traumatology. In the past, conservative therapy in the form of interjaw fixation was favored and is currently being replaced in some cases by surgical interventions. Despite this, conservative therapy has an irreplaceable role in the traumatology of the facial skeleton, especially in non-dislocated fractures of the articular process of the mandible or intra-articular fractures. Indications for splint osteosynthesis of the mandibular process fracture are not yet clearly established and even today they are a source of passionate expert polemics, unequivocal recommendations regarding conservative or surgical treatment are missing. We present a group of 64 patients with mandible articular process fracture who were treated conservatively or surgically and then followed after 2, 6 and 12 months. The monitored parameters included the occurrence of sound phenomena in the temporomandibular joint at function, the range of opening of the mouth in millimeters (mm), mandible protrusion (mm), mouth opening symmetry and of course the patient‘s satisfaction with the state of health. The results show that correctly indicated and applied therapy followed by careful rehabilitation has an invaluable benefit for the patient and minimizes the risk of complications.
Keywords:
mandibular fractures – conservative therapy – surgical therapy – temporomandibular joint
Introduction
Due to its anatomical position, the lower jaw is one of the most exposed parts of the facial skeleton; its injuries account for about 50 % of fractures of the orofacial system [1]. Fractures of the mandible can be divided into fractures of the alveolar process, chin region, mandible body, mandible angle, mandible branch, articular process, muscular process, and unspecified mandible fractures [2]. Approximately 25 –40 % of the mandibular fractures involve a fracture of the articular process and their number increases [5]. This is due to an increase in the frequency of sports injuries, traffic accidents, but also an improvement in diagnostics, which was mainly due to the standard introduction of computed tomography (CT), in the examination algorithm of patients with head injuries, i.e. injuries of facial skeleton [3, 9, 10]. Previously routinely used X-ray examination of the skull does not have the same diagnostic value in the fractures of the articular process of mandible as the CT scan mentioned above and does not provide an ideal overview of the mutual relationship of bone fragments of dislocated fractures. From our point of view, the orthopantomogram (OPG) is also suitable, where the area of the articular process is very well visible. OPG is thus a significant benefit in dislocated fractures, and also allows comparison with the other side of the articular process. About two-thirds of the fractures of the articular processes (APF) occur in men and one-third in women [9]. In males, these fractures occur most frequently in the second and third decades, in females only in the fourth decade. This difference is due to gender-related injuries: in men these are often criminal injuries, while women these are leisure time injuries. In children, the etiology of APF is different than in adults. The most common cause in this period of life is a fall, most often from a bicycle [5].
In clinical examination we observe typical signs of a fracture (i.e. pain, swelling, impaired or lost function, impaired bone continuity) and specific signs, i.e. limited opening of the mouth, deviation of the lower jaw to the side of the broken condyle (Fig. 1). Another symptom is a bite disorder, both subjectively perceived by the patient and objectively diagnosed, especially in fractures with dislocation of fragments. Pain is manifested by palpation preauricularly, in the area of tension or pressure on the mandible, at the angle of the mandible. Furthermore, palpation in the external auditory canal is painful, where the laceration of the skin of the external auditory canal by bone fragmentation is sometimes apparent in dislocated fractures of the articular process of the mandible.
Fig. 1. Patient with a fracture of articular recess of mandible and open bite 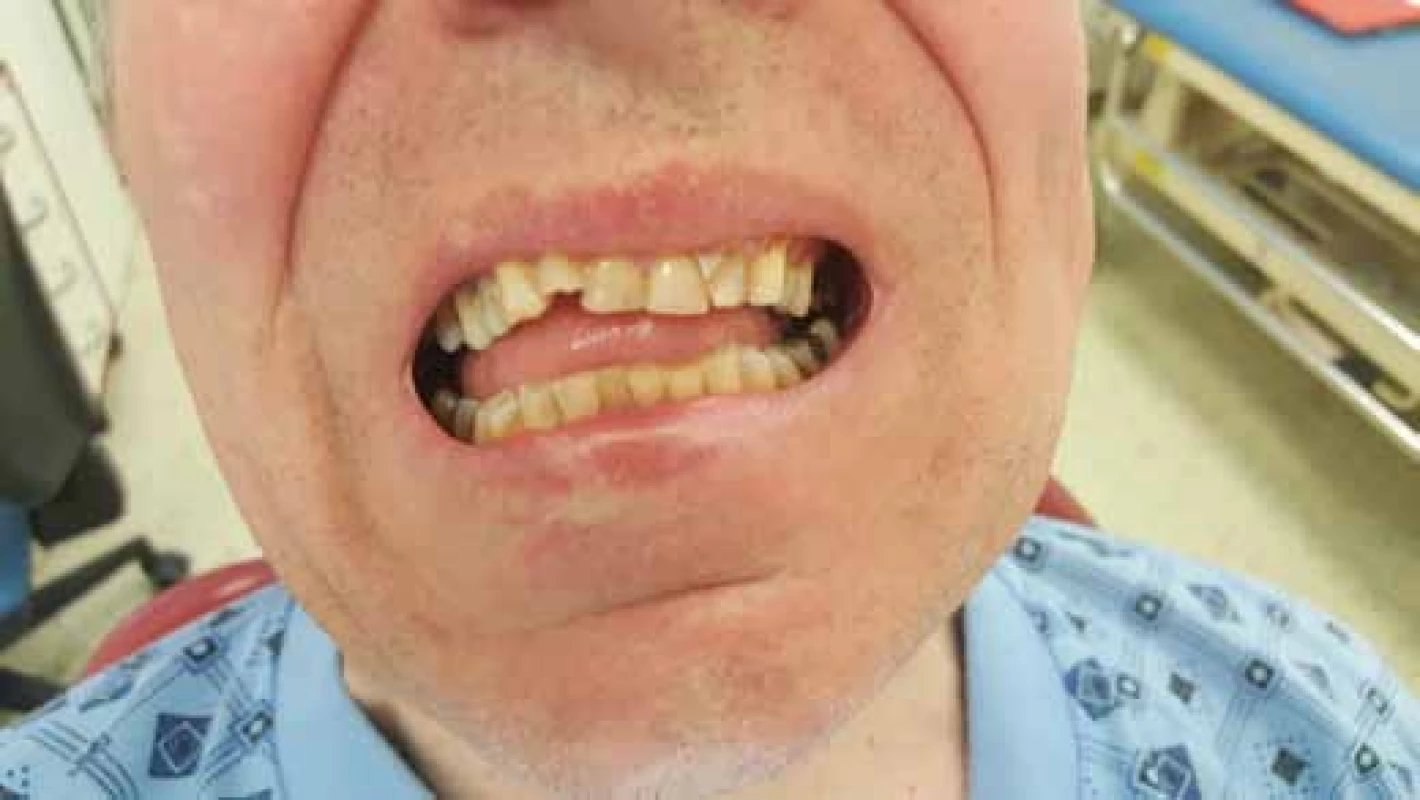
In the treatment of fractures of the articular processes in adults it is possible to adopt two approaches: conservative with a period of inter-jaw fixation followed by functional therapy and rehabilitation (Fig. 2), or surgically with open reduction with/without inter-jaw fixation (Fig. 3). When choosing the most appropriate treatment we consider several factors: the size and quantity of the fracture lines, whether it is a one - or two-sided fracture, the condition of dental arches in the upper and lower jaw and their relationship, the effect of the affected temporomandibular joint (TMJ) to the lower jaw movements and chewing system, degree and direction of dislocation of fragments, general health condition of the patient, presence of other facial fractures, and last but not least, experience and habits of the surgeon and clinical workplace concerned [4, 6, 7, 8].
Fig. 2. Patient with non-dislocated fracture of mandibular articular process with fixed interjaw fixation (conservative therapy) 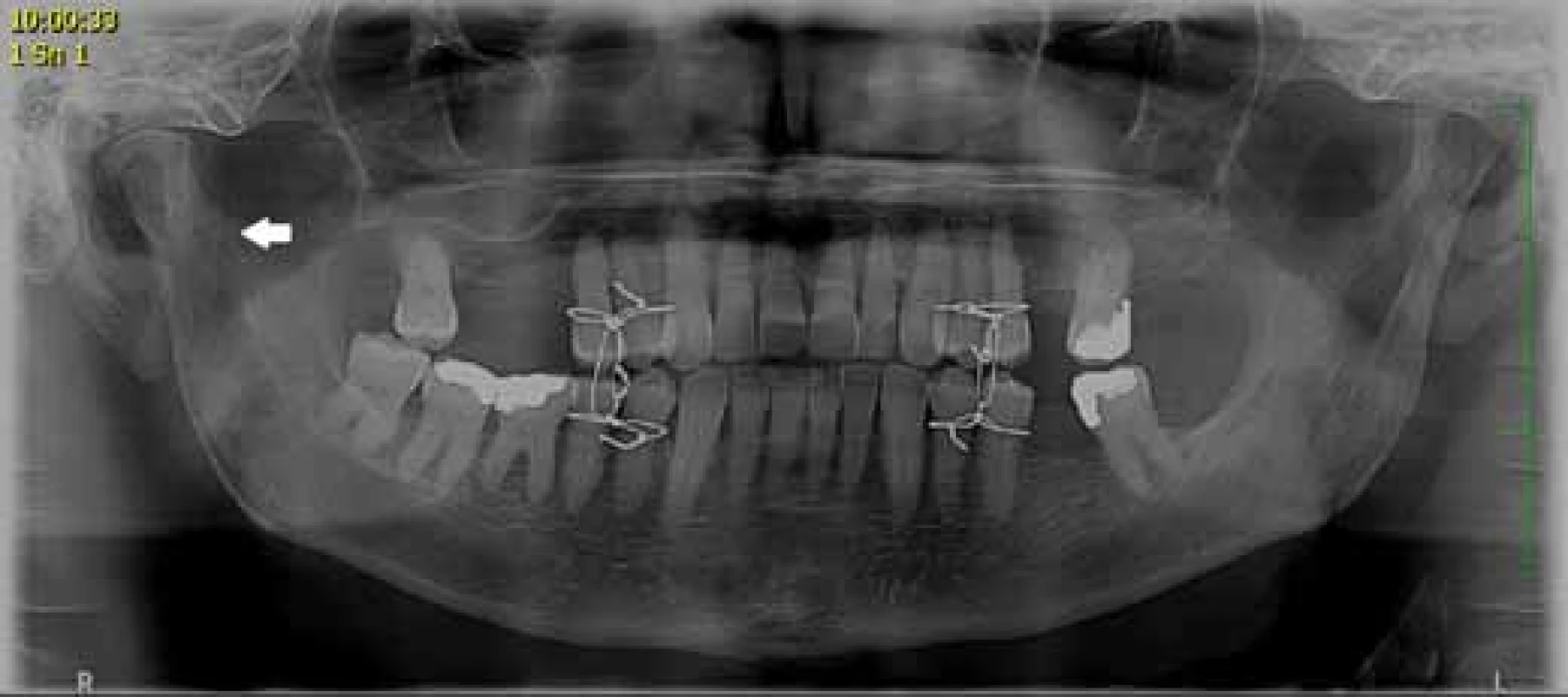
Fig. 3. Patient with fracture of articular process of left mandible, which was treated with osteosynthesis (surgical therapy) 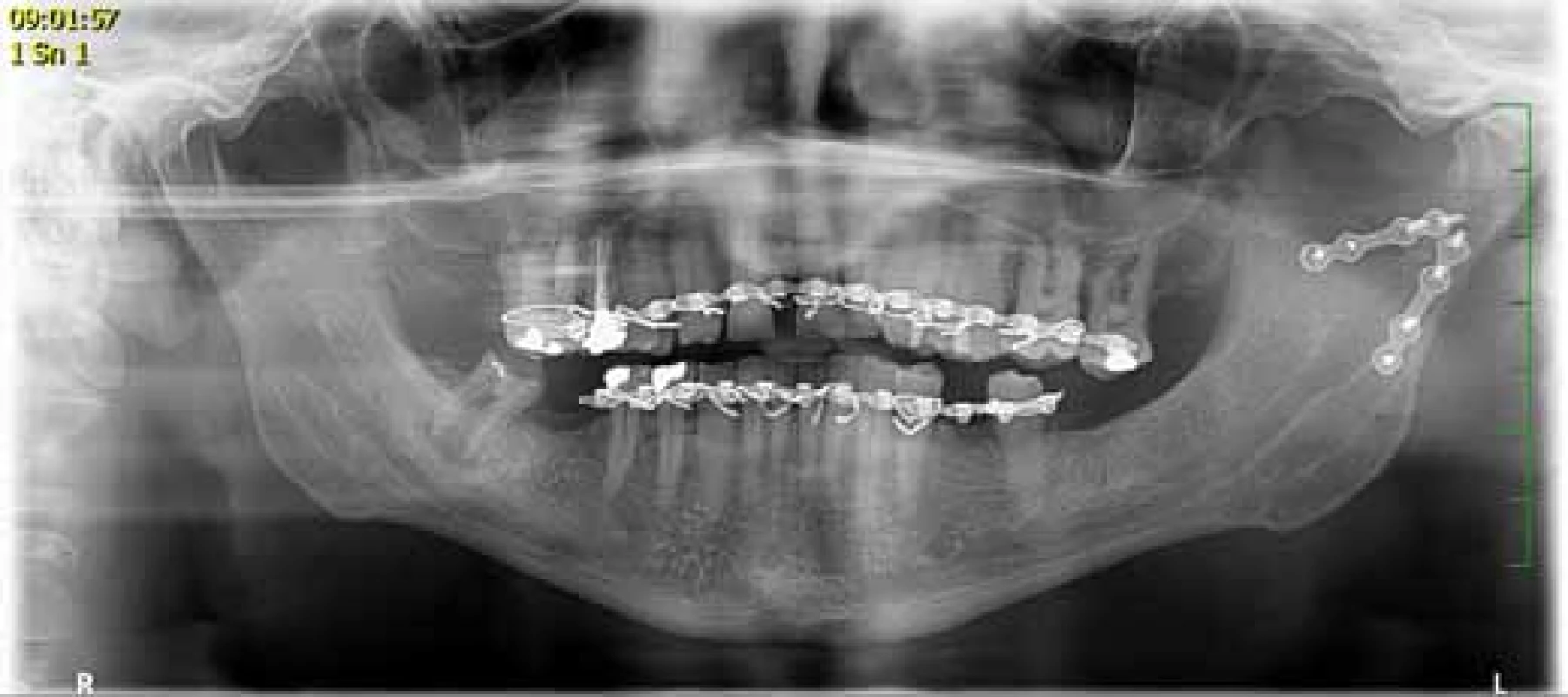
The aim of our publication is to compare conservatively and surgically treated patients with APF and their subsequent convalescence and extent of lower jaw movements after fracture treatment.
Material and methodology
This is a retrospective study involving 64 patients with APF treated at the Department of Oral Jaw and Facial Surgery, University Hospital in Ostrava in 2014. These patients were followed up for 2, 6 and 12 months after the injury at our outpatient clinic, where the following parameters were monitored: sound phenomena in temporomadibular joint in function, range of opening of the mouth in millimeters (mm), lower jaw protrusion (mm), mouth opening symmetry, and, of course, the patient‘s satisfaction with his or her health condition. The results were then statistically evaluated.
Results
Of 64 patients, 46 patients (72 %) underwent conservative treatment and 18 (28 %) underwent surgical treatment. Of the total of 64 patients, 21 (33 %) had a right-sided fracture, 27 (42 %) had a left-sided fracture and 16 (25 %) had a double-sided fracture. The mean period of inter-jaw fixation was 21 days, the standard deviation of the fixation period was 12 days. A quarter of patients had fixation period of less than 12 days, a quarter of patients longer than 30 days. Half of the patients had a fixation period of up to 17 days. The observed differences between fixation times in the compared groups of patients cannot be described as statistically significant at the significance level of 0.05 (Mann-Whitney test).
Occurrence of sound phenomena after treatment (fixation)
At the two-month follow-up, 35 (73 %) of 48 patients who received conservative treatment and 14 (87 %) of 16 patients who received surgical treatment were free of sound phenomena. At 12 months after discontinuation of treatment, 46 (96 %) of 48 patients who received conservative treatment and 15 (94 %) of 16 patients who received surgical treatment were free of sound phenomena. The observed difference in the success rate of conservative and surgical treatment is not statistically significant at the significance level of 5 % (Wilson‘s homogeneity test of two binomial distributions).
Opening range (mm)
The development of the opening range at 2, 6 and 12 months was 38, 45 and 44 mm in the conservatively treated patients, 37, 39 and 45 in the surgically treated patients. The observed differences between the conservative and surgical methods are not statistically significant at the significance level of 5 % (Mann-Whitney test).
Graph 1. Comparison of opening range (mm) for patients treated by conservative and surgical methods 
Protrusion
The development of protrusion (mm) after 2, 6 and 12 months was 5, 5 and 5 mm in conservatively treated patients, 2, 3.5 and 2 in surgically treated patients. (Chart 2). At a 2-month follow-up examination, the average protrusion is statistically significantly (at a significance level of 5 %) lower in patients with surgical treatment (Mann-Whitney test). The observed differences between the conservative and surgical treatment methods at follow-up examinations at 6 and 12 months are not statistically significant at the significance level of 5 % (Mann-Whitney test).
Graph 2. Comparison of protrusion (mm) for patients with conservative and surgical treatment 
Mouth opening symmetry
At 6 months follow-up visit, mouth opening asymmetry was diagnosed in 8 (17 %) of 48 patients with conservative treatment and in 4 (25 %) of 16 patients with surgical treatment. At 12 months follow-up visit, the incidence of mouth opening asymmetry decreased to 3 (6 %) out of 48 patients treated conservatively and 2 (13 %) out of 16 patients treated surgically. The observed differences between the occurrence of mouth opening asymmetry in patients treated conservatively and surgically are not statistically significant at the significance level of 5 % (Wilson‘s homogeneity test of two binomial distributions).
Patient satisfaction
At the 2-month follow-up visit, 42 (87 %) of 48 patients treated conservatively and 14 (87 %) treated surgically expressed satisfaction with the state of health. At follow-up visit at 6 months, the number of patients satisfied with the health condition increased to 46 (96 %) in the conservatively treated group and 15 (94 %) in the surgically treated group. At the 12-month follow-up visit, in the group of conservatively treated patients the number of satisfied patients decreased to 44 (92 %), in the group of surgically treated patients the number of satisfied patients remained unchanged. The observed differences in satisfaction between patients with conservative and surgical treatment are not statistically significant at the significance level of 5 % (Wilson‘s homogeneity test of two binomial distributions).
Discussion
In the past, conservative treatment was favored in almost all patients with articular process fracture. Surgical treatment was the second choice method, due to the frequent occurrence of peroperative and postoperative complications [1].
In our department we indicate surgical therapy in adult patients with bilateral APF, as well as in unilateral fractures in case of dislocation of “to contraction” fragments by more than 5 mm, or in case of cranial fragment axis deviation greater than 30 degrees from the original position. Surgical therapy is also favored for toothless jaws and in patients with bite disorder or facial asymmetry. Conservative therapy is indicated in the case of undislocated unilateral FPA, when the patient does not have a broken bite and in the case of intra-articular FPA. The indication criteria for FPA surgical therapy in our department are similar to those reported in the current literature [11, 12]. Deviations can be observed in views of the dislocation angle and the length of the shortening of the mandible branch. According to various authors, the limit values for the indication for surgical therapy range from 10 to 50 degrees for the dislocation angle and from 1 to 5 mm for the branch shortening [4, 6, 7, 8].
Our results show that the outcome of the mouth opening range, protrusion and movement symmetry of both jaw joints are - in compliance with the above mentioned indication criteria - comparable in both methods. Haug and Assael, who compared these parameters in 10 surgically treated and 10 conservatively treated patients [13], came a very similar conclusion, however, in patients treated surgically, a 6-month follow-up visit showed a significantly improved result in functional values. This group of patients also reported less pain and increased comfort.
According to the study by Santler et al. involving 234 patients with articular process fracture treated with the open or closed method, the only significant difference was subjective discomfort [14]. However, the patients undergoing surgical therapy were experiencing greater pain with their mouths open to a maximum, and therefore the authors recommended using this method only in significant dislocations of the condylar process [14]. In the group of our patients the subjective discomfort was comparable in both forms of therapy.
There are currently no clear criteria for indicating conservative or surgical treatment. For a long time, the preferred method of treatment was conservative [15], but in recent years surgical treatment has also come to the fore. However, the authors agree that therapy must be indicated on a case-by-case basis and that the experience of each surgeon must also be taken into account [16]. Temporomandibular joint belongs to anatomical units with difficult surgical approach. The complication is the risk of postoperative damage to the facial nerve and parotid gland with subsequent paresis of facial mimic muscles or salivary fistula. Reposition of a dislocated fragment can also be quite difficult. Therefore, the surgical therapy should be performed by an experienced surgeon who can minimize or resolve possible complications.
Conclusion
Therapy of fractures of the condylar process of the mandible is one of the controversial topics in maxillofacial traumatology and the success of therapy requires the cooperation of the surgeon, the physiotherapist and of course the patient. For best results, timely mobilization after treatment, whether conservative or surgical, consistent adherence to the postoperative regimen, and the most accurate anatomical reconstruction of the fragments, which in some cases can only be achieved by surgical intervention, are important. Long-term studies are currently lacking to show the different benefits of conservative and surgical treatment. Another problem can be an objective and subjective evaluation of the extent of mouth opening and their statistical evaluation. Therefore, further research is needed to help answer this question.
This article was created with the support of MH CR – RVO – UHO/2017
MUDr. Jan Štembírek
Zdroje
1. Abdel-Galil, K., Loukota, R. Fractures of the mandibular condyle: evidence base and current concepts of management. Br J Oral Maxillofac Surg. 2010.
2. Audigé, L., Prein, J. The comprehensive AOCMF classification system for fractures of the craniomaxillofacial skeleton. Craniomaxillofacial Trauma & Reconstruction. 2014, 7, 1, S1–S140.
3. Kisnisci, R. Management of fractures of the condyle, condylar neck, and coronoid process. Oral Maxillofac Surg Clin North Am. 2013, 25, 573–590.
4. Pilling, E., Eckelt, U., Loukota, R. et al. Comparative evaluation of ten different condylar base fracture osteosynthesis techniques. British Journal of Oral & Maxillofacial Surgery, 2010, 48, 527–531.
5. Sawazaki, R., Lima, jr. SM., Asprino, L. et al. Incidence and Patterns of Mandibular Condyle Fractures. Journal of Oral and Maxillofacial Surgery. 2010, 68, 1252–1259.
6. Shiju, M., Rastogi, S., Gupta, P. et al. Fractures of the mandibular condyle-Open versus closed-A treatment dilemma. J Craniomaxillofac Surg. 2015, 43, 448–451.
7. Rastogi, S., Sharma, S., Kumar, S. et al. Fracture of mandibular condyle - to open or not to open: an attempt to settle the controversy. Oral Surg Oral Med Oral Pathol Oral Radiol. 2015, 119, 608–613.
8. Vesnaver, A., Ahčan, U., Rozman, J. Evaluation of surgical treatment in mandibular condyle fractures. J Craniomaxillofac Surg. 2012, 40, 647–653.
9. Zachariades, N., Mezitis, M., Mourouzis, C. et al. Fractures of the mandibular condyle: A review of 466 cases. Literature review, reflections on treatment and proposals. Journal of Cranio-Maxillofacial Surgery. 2006, 34, 421–432.
10. Zhou, H., Liu, Q., Cheng, G. et al. Aetiology, pattern and treatment of mandibular condylar fractures in 549 patients: A 22-year retrospective study. Journal of Cranio-Maxillofacial Surgery. 2013, 41, 34–41.
11. Al-Moraissi, EA, Ellis, E. Surgical treatment of adult mandibular condylar fractures provides better outcomes than closed treatment: a systematic review and meta-analysis. J Oral Maxillofac Surg. 2015, 73, 482–493.
12. Yao, S., Zhou, J., Li, Z. Contrast analysis of open reduction and internal fixation and non-surgical treatment of condylar fracture: a meta-analysis. J Craniofac Surg. 2014, 25, 2077–2080.
13. Haug, RH, Assael, LA. Outcomes of open versus closed treatment of mandibular subcondylar fractures. J Oral Maxillofac Surg. 2001, 59, 370–375.
14. Santler, G., Kärcher, H., Ruda, C. et al. Fractures of the condylar process: surgical versus nonsurgical treatment. J Oral Maxillofac Surg. 1999, 57, 392–397.
15. Brandt, MT, Haug, RH. Open versus closed reduction of adult mandibular condyle fractures: a review of the literature regarding the evolution of current thoughts on management. J Oral Maxillofac Surg. 2003, 61, 1324–1332.
16. Niezen, ET, Bos, RRM, Minnen, B. et al. Fractures of the mandibular condyle: A comparison of patients, fractures and treatment characteristics between Groningen (The Netherlands) and Dresden (Germany). J Craniomaxillofac Surg. 2018, 46, 1719–1725.
Štítky
Chirurgie všeobecná Traumatologie Urgentní medicína
Článek vyšel v časopiseÚrazová chirurgie
Nejčtenější tento týden
2018 Číslo 4- Metamizol jako analgetikum první volby: kdy, pro koho, jak a proč?
- Stillova choroba: vzácné a závažné systémové onemocnění
- Hojení análních fisur urychlí čípky a gel
- Jak souvisí postcovidový syndrom s poškozením mozku?
- Cinitaprid – v Česku nová účinná látka nejen pro léčbu dysmotilitní dyspepsie
-
Všechny články tohoto čísla
- Non-unions after intramedullary nailing of fractures of the humeral diaphysis
- Conservative and surgical treatment of fractures of articular process of mandible in adults
- Therapeutic results of acromioclavicular dislocations by means of a hook plate and tension wire band
- INTRA-ARTICULAR DISLOCATION FRACTURES OF THE MIDDLE PHALANX BASE - CASE REPORTS OF INCORRECT TREATMENT PROCEDURES, CURRENT TREATMENT CONCEPTS
- Omluva autorům článku publikovaného v čísle 3/18 Úrazové chirurgie, vydaného ke dni 30. 6. 2019
- Úrazová chirurgie
- Archiv čísel
- Aktuální číslo
- Informace o časopisu
Nejčtenější v tomto čísle- INTRA-ARTICULAR DISLOCATION FRACTURES OF THE MIDDLE PHALANX BASE - CASE REPORTS OF INCORRECT TREATMENT PROCEDURES, CURRENT TREATMENT CONCEPTS
- Non-unions after intramedullary nailing of fractures of the humeral diaphysis
- Therapeutic results of acromioclavicular dislocations by means of a hook plate and tension wire band
- Conservative and surgical treatment of fractures of articular process of mandible in adults
Kurzy
Zvyšte si kvalifikaci online z pohodlí domova
Autoři: prof. MUDr. Vladimír Palička, CSc., Dr.h.c., doc. MUDr. Václav Vyskočil, Ph.D., MUDr. Petr Kasalický, CSc., MUDr. Jan Rosa, Ing. Pavel Havlík, Ing. Jan Adam, Hana Hejnová, DiS., Jana Křenková
Autoři: MUDr. Irena Krčmová, CSc.
Autoři: MDDr. Eleonóra Ivančová, PhD., MHA
Autoři: prof. MUDr. Eva Kubala Havrdová, DrSc.
Všechny kurzyPřihlášení#ADS_BOTTOM_SCRIPTS#Zapomenuté hesloZadejte e-mailovou adresu, se kterou jste vytvářel(a) účet, budou Vám na ni zaslány informace k nastavení nového hesla.
- Vzdělávání



