-
Články
- Vzdělávání
- Časopisy
Top články
Nové číslo
- Témata
- Kongresy
- Videa
- Podcasty
Nové podcasty
Reklama- Kariéra
Doporučené pozice
Reklama- Praxe
Splint rib osteosynthesis: our experience
Authors: Lucie Sochorová 1; Lubomír Kopp 2,3; Vilém Malý 1; Petra Pavlíková 1; Ivan Staněk 1
Authors place of work: Oddělení hrudní chirurgie, Masarykova nemocnice, Ústí nad Labem, 2Klinika úrazové chirurgie, Masarykova nemocnice, Ústí nad Labem, 3Ústav anatomie, 2. lékařská fakulta Univerzity Karlovy, Praha Masarykova nemocnice o. z., Krajská zdravotní a. s., krajská 1
Published in the journal: Úraz chir. 27., 2020, č.2
Summary
Aim of the work: To present indications, surgical technique, complications and mid-term results on a set of prospectively monitored patients with performed osteosynthesis of multiple rib fractures.
Material and methods: In the period from January 2018 to May 2019, we performed osteosynthesis in 15 patients who were followed for at least 6 months. The indication was a multiple rib fracture with instability of the chest wall, a serial fracture of 3 and more ribs with a gross deformity of the chest wall and intrathoracic pathology requiring surgical procedure, in combination with one or more broken ribs. We used an innovated system of rib splints of a Czech manufacturer for the osteosynthesis. The average age of patients was 58. The most frequent mechanism of injury was a high-energy injury (in 10 cases). Out of the associated injuries, skeleton fractures in the area of chest and upper limbs in a total of eight patients were the most frequent ones. Traumatic hemothorax was present in 13 patients, pneumothorax in seven. Contusion of the lungs was reported in seven patients, and six multiple rib fractures were present in the set. Bilateral rib fractures occurred in six patients.
Results: The time from injury to operating procedure ranged from 2 hours to 13 days. Most often, we performed osteosynthesis of 3 ribs using 4 splints. The average length of stay at the intensive care unit was 5.2 days. Surgical wounds healed primarily. As to early postoperative complications, we reported hemothorax in one case and fluidothorax in one case. Two patients were treated postoperatively for bronchopneumonia. Bone healing was achieved in all patients after 24 weeks.
Discussion: The advantage of surgical stabilization is reduction of the time of artificial pulmonary ventilation including reduction in the incidence of related complications. In a complex chest injury, we consider it important to combine surgical stabilization of the ribs with the shoulder girdle osteosynthesis.
Conclusion: We recommend surgical treatment of multiple rib fractures in multiple rib fractures, serial fractures with chest wall deformity, and in procedures associated with the treatment of an intrathoracic pathology. Splint osteosynthesis with innovated Judet-type rib splints is comfortable and safe and results in bone healing achieved.
Keywords:
complications – Rib osteosynthesis – indications – innovated rib splints
Introduction
Multiple rib fractures are one of the most common types of chest injuries. In high-energy polytrauma injuries, they are associated with high morbidity and mortality [1, 15]. The most frequent causes include ventilation disorders due to pain, limitation of respiratory volume, complications of long-term artificial pulmonary ventilation, lung infection, or general superinfection [3, 7, 11]. In the recent 10 years, significant development of surgical techniques for stabilization of multiple rib fractures [13, 16] has been reported. Systems of sufficiently rigid but shapeable locking splints ensuring stable fixation of rib fractures have been introduced into clinical practice. Through the development in this field, innovation of Judet-type splints resulted in development of a purely domestic system available to most of our sites [9, 14].
The aim of the authors is to present indications, surgical technique, complications, and mid-term results on their own set of prospectively monitored patients with performed osteosynthesis of multiple rib fractures.
Material and method
The author‘s site is a part of the Level 1 trauma centre with approximately 150 patients with ISS over 16 treated annually. In the period from January 2018 to May 2019, we treated a total of 116 patients with multiple rib fractures (3 and more) and out of this number we performed osteosynthesis in a total of 15 patients (12.9 %). In all of them, we followed the following factors prospectively: age, gender, trauma mechanism, localization of rib fractures and the degree of their dislocation, associated intrathoracic injuries and associated injuries of other organs and systems. Also the time from injury to surgical treatment, the number of patients with simultaneous revision of the thoracic cavity, the number of osteosynthesized ribs and splints used, the length of stay in the ICU, the need for artificial pulmonary ventilation, and the overall duration of hospitalization. We also monitored the occurrence of complications in terms of early and intrathoracic infections, bone healing disorders, and long-term pain. The minimum follow-up period was 6 months (6-23 months).
We performed a planning CT imaging with 3D rib reconstruction in all patients (Fig. 1). Indications for osteosynthesis in our set included multiple rib fracture with chest wall instability, serial fracture of 3 or more ribs with a dislocation causing chest wall deformity (Fig. 2), and intrathoracic pathology in the sense of hemo - or pneumothorax, requiring surgical intervention, in combination with one or more broken ribs (so-called on the way out fixation) (Fig. 3). Another indication at our site is the clinically manifested false joint in the area of the ribs. However, this group of patients is not a part of the monitored set in order to maintain homogeneity. We operated exclusively surgically achievable fractures in the area of diaphysis of ribs 3 to 9 (according to the classification of the AO Working Group on Osteosynthesis for 16.1-2.3-9.2), with the distance of the fracture line from the costotransverse articulation being at least 3 cm.
Fig. 1. CT 3D reconstruction of serial rib 3 - 10 fracture on the left with a multiple fracture of ribs 3 - 6 causing instability of the chest wall 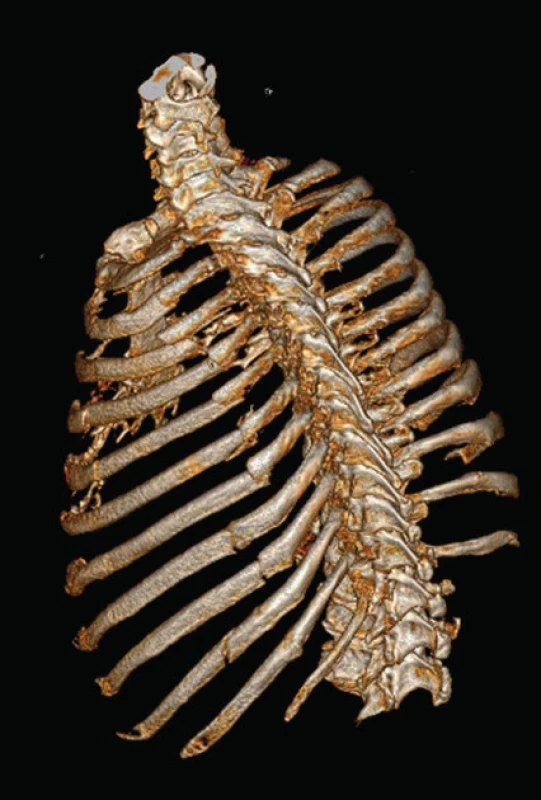
Fig. 2. CT 2D coronal reconstruction of serial fracture of the ribs on the right with a gross chest wall deformity 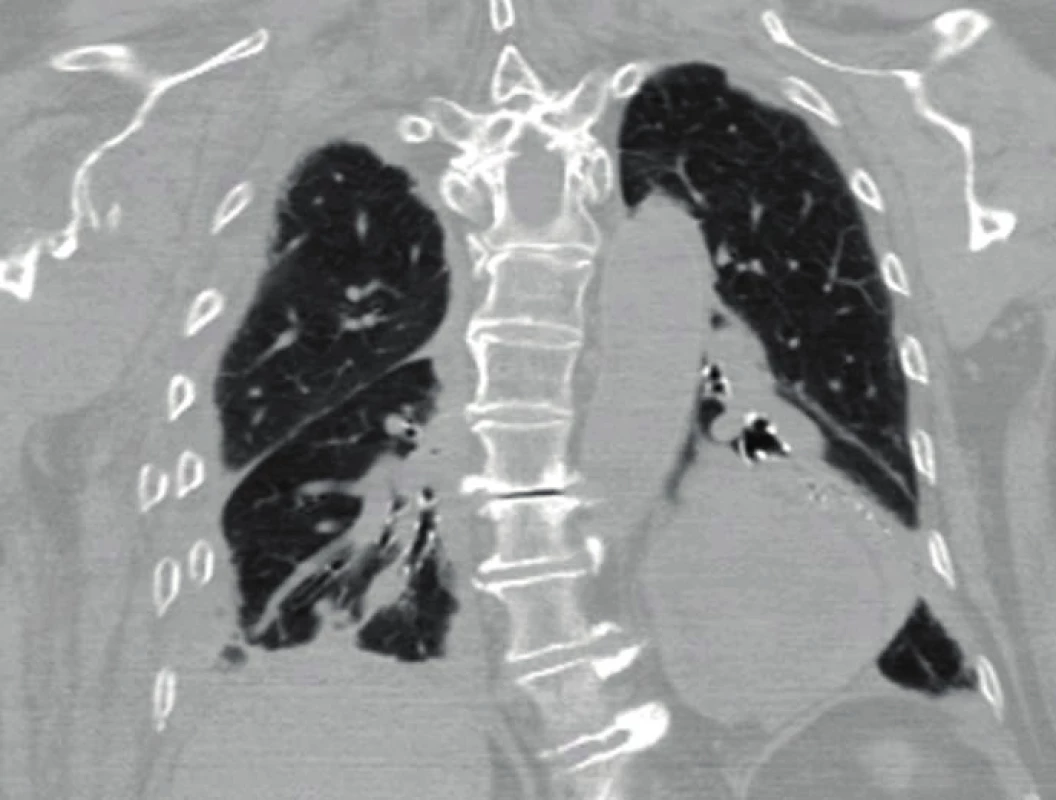
Fig. 3. CT transverse projection of the progressive hemothorax on the left in a patient with a serial rib fracture 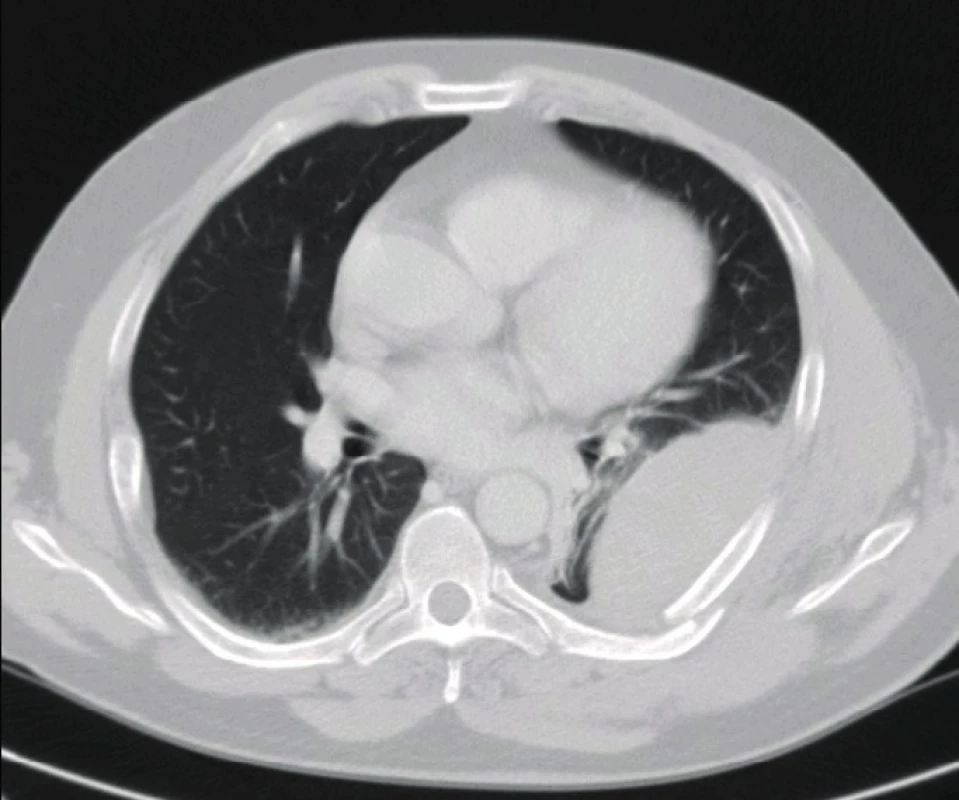
We operated all patients in lateral position on the healthy side; we elected the surgical approach with regard to the localization of fracture lines, most often using antero - or posterolateral thoracotomy. With regard to soft tissues, we performed muscle dissection only to the necessary extent (Fig. 4); we used techniques of MIPO osteosynthesis for suitable fractures. We also combined a thoracoscopic revision of the thoracic cavity with subsequent osteosynthesis.
Fig. 4. Sparing dissection of muscles for rib splint application, limiting postoperative soreness 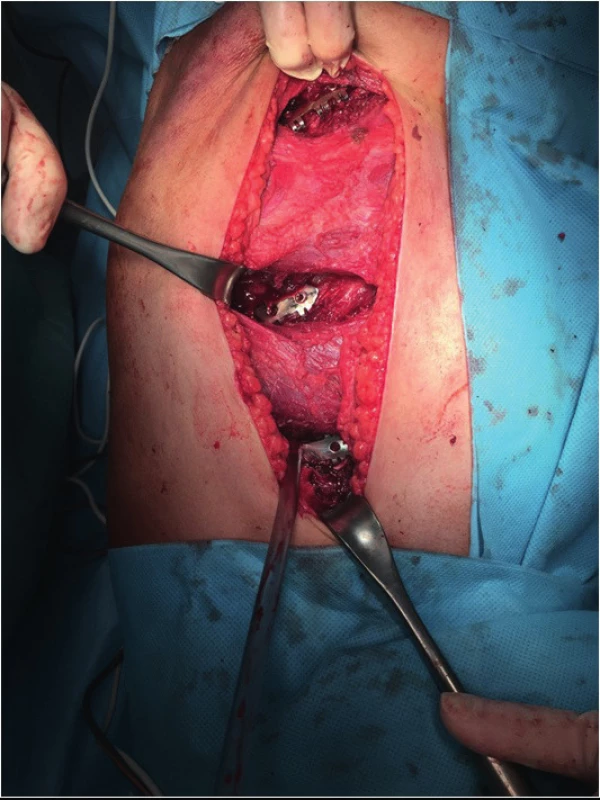
Fig. 5. Application of fixation clips in the area of lower edge of the rib in subperiosteal position in order to reduce compression of the neurovascular bundle 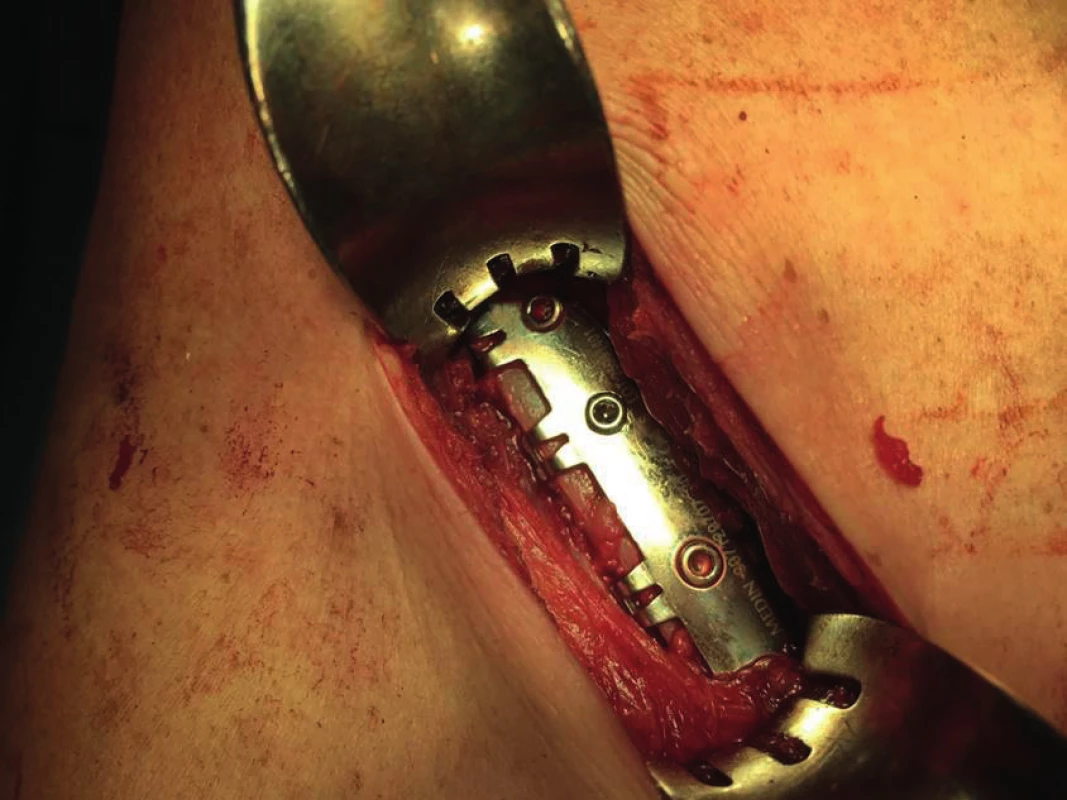
To fix the ribs, we used an innovated system of rib splints (Medin company, Nové Město na Moravě), featuring locking screws, modified fixing clips to anchor around the ribs, and a complete instrumentation to form and fix the splints to the skeleton. The splints are supplied in lengths of 40 – 155 mm, which allowed for biomechanically advantageous bridging of segmental fractures of the ribs with one implant. In order to prevent post-operation neuralgia, we applied fixation clips in the lower rib area in subperiosteal location in selected patients (deferred procedure, haemodynamic stability).
Out of the 15 patients operated, there were 12 men and 3 women. The average age of patients was 58 (35–80 years). The mechanism of injury was a high-energy injury in 10 cases (67 %) and a low-energy injury in 5 cases (33 %). In high-energy injuries, 8 cases were caused by car - or motorcycle accidents, the remaining 2 patients suffered a direct impact in the area of the rib cage (falling tree impact, cow kick). As to low-energy injuries, 3 patients were injured after falling from a standing height, and 2 from a height of less than 2 meters.
Out of the associated injuries, skeleton fractures in the area of chest and upper limbs in a total of eight patients (53 %) were the most frequent ones. Clavicle was broken five times (always with the dislocation of fragments), blade three times, sternum once, humerus once. Craniotrauma occurred in 3 patients (20 %) in a form of brain contusion or intracranial bleeding. Cavity injuries were suffered by 2 patients (13 %); in one case it was a spleen rupture, in the other one it was a contusion of pancreas. We also reported a trauma rupture of the diaphragm in two cases (13 %), as well as facial skeleton injuries. Three patients suffered fractures of the transverse vertebral processes and one compression fracture of the vertebra. Associated injuries were combined; chest trauma without additional injuries occurred in four patients (27 %) only.
Traumatic hemothorax was present in 13 patients (87 %), pneumothorax in seven patients (47 %); in one case it was tension pneumothorax with the need for urgent thoracic drainage at the acute admission department. Contusion of pulmonary parenchyma was reported on the admission in 10 patients (67 %), of which seven were minor contusion foci; in three cases we observed a massive contusion (over 30 %), which in one patient was also combined with massive haemorrhage into pulmonary parenchyma. In three patients, contusion occurred on both sides. There were six multiple rib fractures (40 %) in the set. Bilateral rib fractures were observed in six patients (40 %) as well. The localization and number of injured ribs are indicated in Table 1.
Tab. 1. Localization and type of rib injury in the set of patients 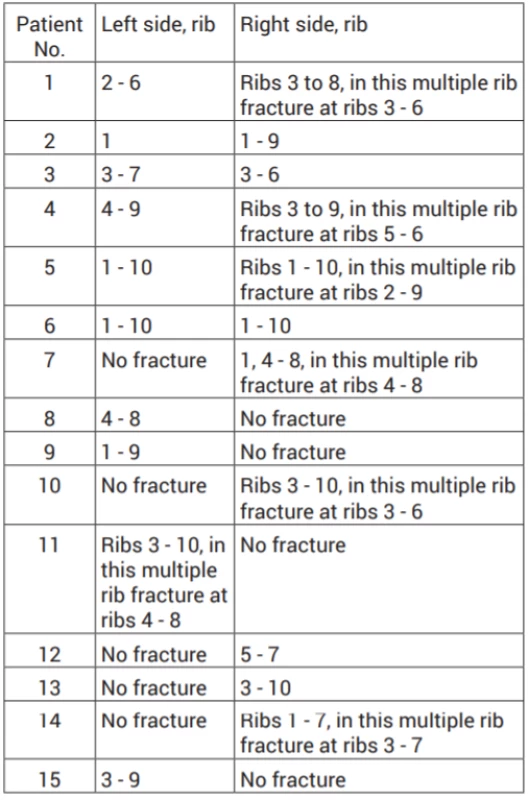
The time from injury to surgery ranged from 2 hours to 18 days. Six patients (40 %) underwent surgery within 24 hours from the accident, another six (40 %) within 4 days.
Results
We performed rib osteosynthesis in 8 patients (53 %) in a form of “on the way out fixation” as a part of the treatment of intrathoracic pathology associated with injury (most frequently it was a progressive hemothorax). In four patients (26 %), the reason for surgical intervention was the chest wall instability in a multiple rib fracture, and in three (20 %) it was a multiple dislocated rib fracture with a chest wall deformity. Concurrent revision of the chest cavity was performed in all 15 patients, using video thoracoscopic method in one of them. Simultaneously with the revision of the chest cavity, we performed the treatment of pulmonary parenchyma laceration in five patients (33 %) and diaphragm suture in two patients (13 %). Most often, we performed osteosynthesis on 3 ribs (1–4) using 4 splints (1–5). As a part of the treatment of complex chest injury with shoulder girdle instability (dislocated fracture of the clavicle), splint osteosynthesis of the clavicle simultaneously with primary treatment of the rib fracture was performed, in cooperation with traumatologists, in 4 of 5 patients affected by this condition.
The average length of stay at the intensive care unit was 5.2 days (1–16 days). The condition of six patients (40 %) required artificial pulmonary ventilation with an average duration of 4.6 days (1–14 days) after the procedure. The average duration of hospitalization was 10.5 days (2–17 days). However, part of the patients was then transferred to a lower site to finish the treatment. One patient died of the second post-trauma day due to consequences of hemorrhagic shock; one patient died on the seventh post-trauma day due to consequences of a septic shock with MODS and SIRS due to severe polytrauma.
Surgical wounds of the other patients healed primarily. As to early postoperative complications, we observed a protracted postoperative hemothorax in one patient without the need for surgical intervention. In one case, we observed the formation of reactive fluidothorax, which was solved by thoracic drainage. Two patients (15 %) were treated postoperatively for bronchopneumonia. Post thoracotomy syndrome in the sense of neuropathic pain lasting for more than three months after the procedure occurred in two patients (15 %). One patient suffered from shoulder pain due to deformity in an untreated fracture of the clavicle.
We monitored bone healing as part of follow-up checks at three and six months with chest X-ray scan, and in indistinct cases with chest CT check-up at six months. The onset of bone healing was observed in all patients after 12 weeks from the injury and it was verified by X-ray or CT scan after 24 weeks. One patient experienced a partial failure of osteosynthesis (locking screw released from the splint) (Fig. 6), which however did not affect the onset of bone healing and did not cause the need for surgical revision.
Fig. 6. Partial failure of osteosynthesis (release of the locking screw – see the arrow), which did not result in mechanical failure of the osteosynthesis; the patient achieved full bone healing, the screw migration did not continue 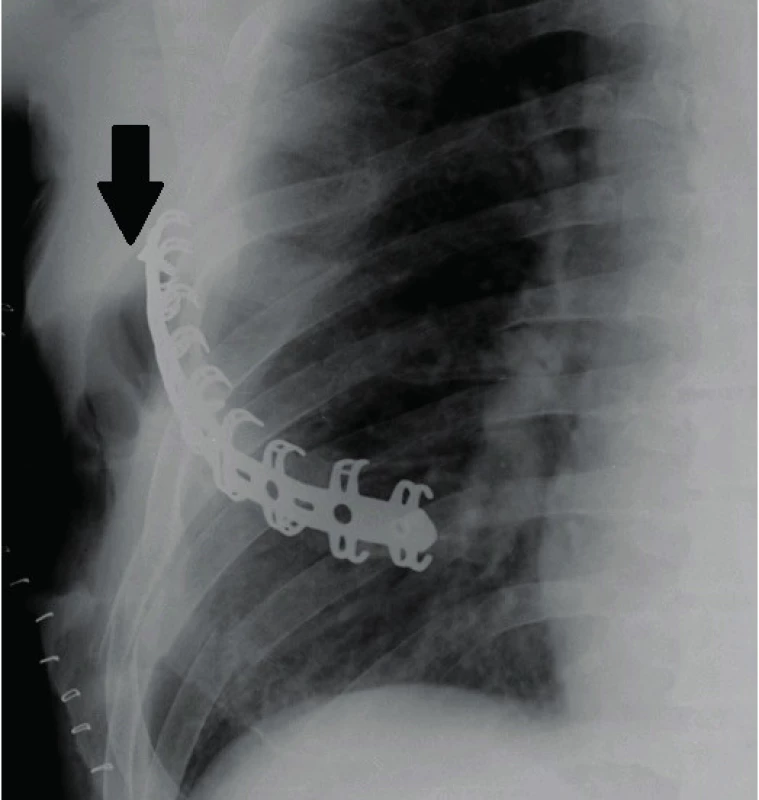
We did not extract osteosynthetic material in any of the patients.
Discussion
Today, most authors consider a multiple rib fracture with instability of the sternum and a serial rib fracture with a pronounced dislocation of fragments (at least the width of the bone), resulting in the chest deformity, an indication for stabilization of multiple rib fractures [11]. Rib osteosynthesis is further performed as „on the way out fixation” upon the revision of the chest cavity due to associated intrathoracic pathology (in the sense of laceration of pulmonary parenchyma, hemo - or pneumothorax, or traumatic rupture of the diaphragm) [1, 5, 15]. Some authors also report age over 45 [2] and strong pain hard to manage by pharmaceuticals [5, 7] as a significant factor. The experience with splint osteosynthesis of the false joints in the chest cage region [4, 6] has already been referred to in case reports as well. Procedures associated with the intrathoracic revision and unstable multiple rib fractures were the dominant indications in our set. Also, a gross chest deformity was the reason for surgical treatment, particularly to prevent the occurrence of long-term consequences (deformity, restriction of respiratory volume, limited of return to original activities) [10].
According to some authors, stabilization of multiple rib fractures is contraindicated in patients with an unstable fracture of the spine and severe craniotrauma [3, 5]. Pieracci et al. does not consider craniotrauma to be an absolute contraindication, taking into account the general condition of the patient [11]. In patients with contusion lung, severe intra-abdominal injury or severe associated skeletal trauma, the indication is relative and depends on the assessment of the patient‘s general condition and the expected benefit of the procedure [1, 11, 13]. In our set, we operated patients with lighter forms of intracranial injury, without impaired consciousness. An extensive contusion of lung tissue was not a contraindication to stabilization either. In all patients, we proceeded individually in the indication, taking into account the severity of the overall injury, taking into account the dynamics of development of the health condition and in cooperation with other specialists (DAR, traumatology).
The advantage of surgical stabilization is the reduction of the time of artificial pulmonary ventilation, including reduction in the incidence of related complications (most often pneumonia or bronchopneumonia and general infection), reduction in the duration of stay at the intensive care unit, a reduction in hospitalization time, reduction in pain, reduction in development of chest deformities, earlier and more frequent return to pre-trauma activities [8, 10, 12, 15]. In our set, the duration of stay at the intensive care unit was comparable to other authors [5, 15, 16]. A low number of only two cases of bronchopneumonia in otherwise severely injured patients indicates the benefit of surgical stabilization of the chest to reduction in the time of artificial pulmonary ventilation and complications associated with the same [8, 12].
Timing of the procedure was early in most patients, which is consistent with other authors [2, 7, 15]. It was based mainly on the associated intrathoracic pathology and dynamics of development of the general health condition. We took into account ventilation problems, especially in cases of unstable multiple rib fractures, and planned the procedure timing according to damage control surgery principles in coordination with other disciplines. In a complex chest injury, we consider it important to combine surgical stabilization of the ribs with the shoulder girdle osteosynthesis, most frequently the fracture of clavicle. Conservative treatment of the fractures of clavicle with simultaneous rib fracture is difficult, since patients do not tolerate traction fixation, and the treatment fails. In one patient where the clavicle was not treated with stable osteosynthesis, a deformity of the shoulder girdle developed in the postoperative period, which also resulted in a worsened chest deformity with adverse functional outcome and restriction of physical activities [3, 10, 12] (Fig. 7a, b).
Fig. 7. a: Defiguration of the shoulder girdle and hemothorax on the left in the absence of treatment of the clavicular fracture, accompanying multiple rib fractures. The patient suffers from severe movement limitation of the upper limb 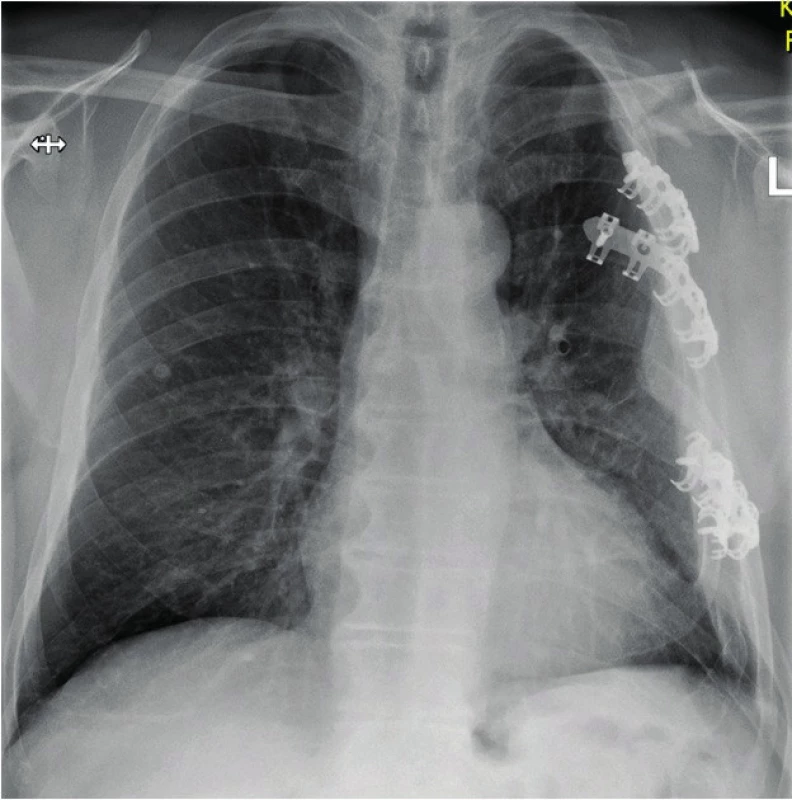
Fig. 7b: Correct chest position with simultaneous stabilization of the shoulder girdle; patient without functional limitation in the chest or upper limb area 
From the point of view of instrumentation, the use of the innovated Judet-type rib splints from the Czech manufacturer was comfortable; the implants themselves were rigid enough but easy to shape. During implantation, we placed fixation clips in subperiosteal area in part of the patients to reduce the irritation of the neurovascular bundle [14]; however, we were unable to remove the pain syndrome completely. The assembly was sufficiently mechanically resistant [7] in all cases and allowed bone healing to be achieved; one case of loosening of the locked screw did not result in any complications.
Conclusion
We can see surgical treatment of multiple rib fractures as beneficial in multiple rib fractures, serial fractures with chest wall deformity, and in procedures associated with the treatment of an intrathoracic pathology. Surgical treatment results in the reduction of acute and chronic morbidity, particularly infection complications and complications associated with artificial pulmonary ventilation. Splint osteosynthesis with innovated Judet-type rib splints is comfortable and safe and results in bone healing achieved.
Zdroje
- BEKS, RB, REETZ, D., DE JONG, M. et al. Rib fixation versus non-operative treatment for flail chest and multiple rib fractures after blunt thoracic trauma: a multicenter cohort study. Eur J Trauma Emerg Surg. 2019, 45, 655–663. ISSN 1863-9933
- BEMELMAN, M., DE KRUIF, MW, BAAL, M. et al. Rib fractures: to fix or not to fix? An evidence-based algorithm. Korean J Thorac Cardiovasc Surg. 2017, 50, 229–234. ISSN 2093-6516
- CAMPOS, JRM, WHITE, TW. Chest wall stabilisation in trauma patiens: why, when and how? J Thorac Dis. 2018, 8, S951–962. ISSN 2072-1439
- DEAN, NC., BOERUM, DH., LIOU, TG. Rib plating of acute and sub-acute non-union rib fractures in an adult with cystic fibrosis: a case report. BMC Research Notes. 2014, 7, 681. ISSN 1756-0500
- HE, Z., ZHANG, D., XIAN, H. et al. The ideal methods for the management of rib fractures. J Thorac Dis. 2019, 11, S1078–1089. ISSN 2072-1439
- JONG, MB., HOUWERT, RM., HEERDE, S. et al. Surgical treatment of rib fracture nonunion: a single center experience. Injury. 2018, 49, 599–603. ISSN 0020-1383
- LARDINOIS, D. General considerations, indications, and potential advantages of chest wall stabilisation, rib fixation, and sternum osteosynthesis in selected patiens after blunt trauma. Shanghai Chest. 2018, 2, 62. ISSN 2521-3768
- MAJEED, FA., ZAFAR, U., IMTIAZ, T. et al. Rib fixation versus conservative management of rib fractures in trauma patiens. J Ayub Med Coll. 2018, 30, 576–584. ISSN 1025-9589
- MAŠEK, M., KITKA, M. Historie stabilizace hrudního koše. Rozhl Chir. 2017, 96, 453–456. ISSN 0035-9351
- OLSÉN, MF, SLOBO, M., KLARIN, L. et al. Physical function and pain after surgical or conservative management of multiple rib fractures – a follow-up study. Scand J Trauma Resusc Emerg Med. 2016, 24, 128. ISSN 1757-7241
- PIERACCI, FM, MAJERCIK, S., ALI-OSMAN, F. Consensus statement: Surgical stabilization of rib fractures rib fracture colloquium clinical practice guidelines. Injury. 2017, 48, 307–321. ISSN 0020-1383
- QIU, M., SHI, Z., XIAN, J. et al. Potential benefits of rib fracture fixation in patiens with flail chest and multiple non-flail rib fractures. Indian J Surg. 2016, 78, 458–463. ISSN 0972-2068
- ŠTĚPÁNKOVÁ, M., VYHNÁNEK, F., GÜRLICH, R., ŠKRABALOVÁ, D. Chirurgická stabilizace hrudní stěny – vývoj metody a současné trendy. Úraz chir. 2017, 25, 129–133, ISSN 1211-7080
- VYHNÁNEK, F., OČADLÍK, M., ŠÁBER, M. Inovovaná žeberní dlaha Judetova typu u nestabilního poranění hrudní stěny. Úraz chir. 2017, 25, 23–27. ISSN 1211-7080
- VYHNÁNEK, F., JÍRAVA, D., OČADLÍK, M., ŠKRABALOVÁ, D. Chirurgická stabilizace u blokové zlomeniny žeber: indikace, technika a výsledky. Acta Chir Orthop Traum Čech. 2015, 82, 303–307. ISSN 0001-5415
- ZHANG, Q., SONG, L., NING, S. et al. Recent advances in rib fracture fixation. J Thorac Dis. 2019, 11, S1070–1077. ISSN 2072-1439
Štítky
Chirurgie všeobecná Traumatologie Urgentní medicína
Článek vyšel v časopiseÚrazová chirurgie
Nejčtenější tento týden
2020 Číslo 2- Metamizol jako analgetikum první volby: kdy, pro koho, jak a proč?
- Nejlepší kůže je zdravá kůže: 3 úrovně ochrany v moderní péči o stomii
- Hojení análních fisur urychlí čípky a gel
- Stillova choroba: vzácné a závažné systémové onemocnění
- Jak souvisí postcovidový syndrom s poškozením mozku?
Nejčtenější v tomto čísle- Supracondylar Fractures of Distal Humerus in Children – Results of Operative Treatment
- Splint rib osteosynthesis: our experience
- Axillary artery injury in low-energy shoulder injury
- Nekrolog Doc. MUDr. František Vyhnánek, CSc.
Kurzy
Zvyšte si kvalifikaci online z pohodlí domova
Autoři: prof. MUDr. Vladimír Palička, CSc., Dr.h.c., doc. MUDr. Václav Vyskočil, Ph.D., MUDr. Petr Kasalický, CSc., MUDr. Jan Rosa, Ing. Pavel Havlík, Ing. Jan Adam, Hana Hejnová, DiS., Jana Křenková
Autoři: MUDr. Irena Krčmová, CSc.
Autoři: MDDr. Eleonóra Ivančová, PhD., MHA
Autoři: prof. MUDr. Eva Kubala Havrdová, DrSc.
Všechny kurzyPřihlášení#ADS_BOTTOM_SCRIPTS#Zapomenuté hesloZadejte e-mailovou adresu, se kterou jste vytvářel(a) účet, budou Vám na ni zaslány informace k nastavení nového hesla.
- Vzdělávání



