-
Medical journals
- Career
Facial Nerve Reconstruction Following Ablative Parotid Surgery - The Ansa Cervicalis Hypoglossal-Facial Anastomosis: A Case Report and Review of Literature
Authors: B. Gál 1; I. Stupka 2; J. Rottenberg 3; J. Hanák 1; P. Urbánková 1; E. Vogazianos 3; D. Slouka 4
Authors‘ workplace: Department of Otolaryngology Head and Neck Surgery, Faculty of Medicine Masaryk University and St. Anne’s University Hospital in Brno 1; Department of Plastic and Reconstructive Surgery, Faculty of Medicine Masaryk University and St. Anne’s University Hospital in Brno 2; Department of ENT, Dorset County Hospital NHS Foundation Trust, Dorchester, UK 3; Department of Otorhinolaryngology, Faculty of Medicine Charles University and University Hospital in Pilsen 4
Published in: Otorinolaryngol Foniatr, 67, 2018, No. 3, pp. 75-78.
Category: Review Article
Overview
Adenoidně cystický karcinom je vzácný, pomalu rostoucí, lokálně agresivní salivární maligní tumor, charakterizovaný infiltrativním růstem a vysokým procentem perineurálního šíření. Primární terapeutickou modalitou pro resekabilní salivární tumory je chirurgická léčba. Při peroperačně prokázané neurální invazi je indikována resekce postižené části větvení lícního nervu. Autoři prezentují modifikaci hypoglosso-faciální anastomózy s využitím ansa cervicalis nervi hypoglossi, jako efektivní techniku rekonstrukce periferního větvení lícního nervu s minimální morbiditou v donorské oblasti.
Klíčová slova:
salivární karcinom, parotidektomie, paréza lícního nervu, rekonstrukce lícního nervu, hypogloso-faciální anastomóza, ansa cevicalis nervi hypoglossi
INTRODUCTION
Parotid gland carcinomas are a relatively rare group of tumours whose primary treatment of choice is a radical surgical resection. The aim of the resection is the safe removal of tumour within negative surgical margins and, if possible dissection of the facial nerve branches and its preservation. If the facial nerve has to be sacrificed due to tumour infiltration or proximity, reconstruction of the facial nerve should be carried out during the same operation, after the resection of the tumour is complete. One of the possible options is the reconstruction using the transposition of the cervical ansa of the hypoglossal nerve (ACNH).
A CASE REPORT
A 77 year old female patient was referred to the Clinic of Otolaryngology, Head and Neck Surgery St. Anne’s Faculty University due to a gradually increasing parotid mass on the right side. On examination the solid mass measuring approximately 4 cm had been localised in the lower pole of the right parotid gland with no objective sign of facial nerve palsy. A CT scan showed a non homogenous, ill-defined infiltrate affecting the distal half of the right parotid glandular parenchyma. No enlarged lymph nodes in the neck were observed. FNA was inconclusive, but salivary adenoid cystic carcinoma with a mixture of tubular and cribriform components was confirmed by open biopsy. A total parotidectomy including an ipsilateral modified subradical neck dissection as a primary treatment, +/ - radiotherapy in case of positive/close margins and/or detection of metastasis was recommended at the Multidisciplinary Team (MDT) meeting.
Perioperatively, the glandular parenchyma was radically resected, and a dissection of part of the facial nerve ramification was performed. The tumour of size 30 x 25 mm was localized in the lower part of the superficial parotid lobe; unfortunately, it had invaded into the cervicofacial trunk (CF) of the facial nerve and to the buccal branch of the temporofacial trunk (TF) (fig. 1). That is why, the CF trunk (including marginal branch and buccal branch B2) and also the buccal branch B1 which was arising from TF trunk had to be sacrificed. Proximal and distal neural stumps were verified as tumour free by frozen section histology. The surgical resection was then completed by modified sub-radical neck dissection involving the II – IV group of lymph nodes. The descending branch of the hypoglossal ansa (ACNH) was dissected and mobilized for later reconstruction, including three branches innervating the strap muscles (fig. 2). The ACNH was transposed to the parotid bed and its three terminal branches were sutured to the peripheral neural stumps of B1, B2 and the marginal branch of the facial nerve using a microsurgical interfascicular suture (fig. 3). Postoperatively, the patient recovered uneventfully. The postoperative pTNM classification was set to pT4 pN1 with detection of early lymph node metastasis in area II. Therefore, postoperative radiotherapy with overall dose of 66 Gy was carried out.
1. Intraoperative photo: Resection of parotid gland parenchyma with tumour mass (TU+PG) invading the buccal branches (B1, B2) and marginal branch (M) of the facial nerve. MT- main trunk, F - frontal branch, Z -zygomatic branch, n.XII - hypoglossal nerve, ACNH- ansa cervicalis n. XII, GAN - great auricular nerve, JIV- internal jugular vein, n.X-vagus nerve, CA- carotid artery, RV - retromandibular vein, SCM - sternocleidomastoid muscle 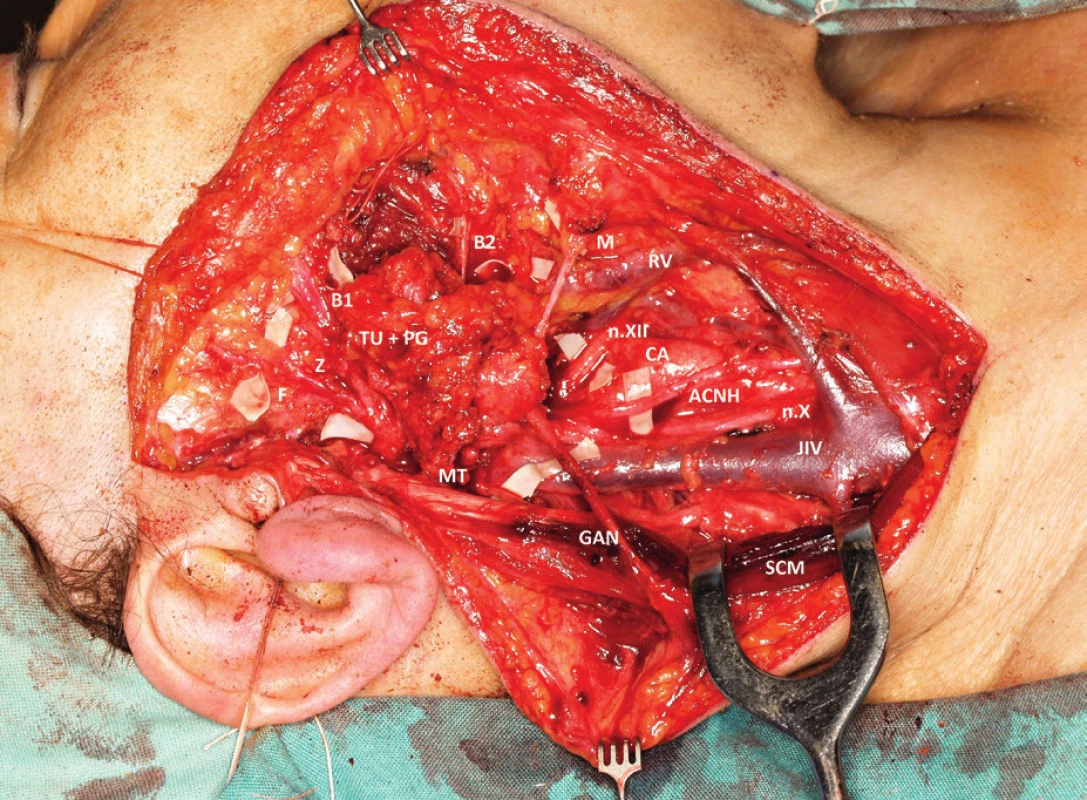
2. Intraoperative photo. Situation after the radical parotidectomy, modified subradical neck dissection and preparation of ansa cervicalis and its branches. 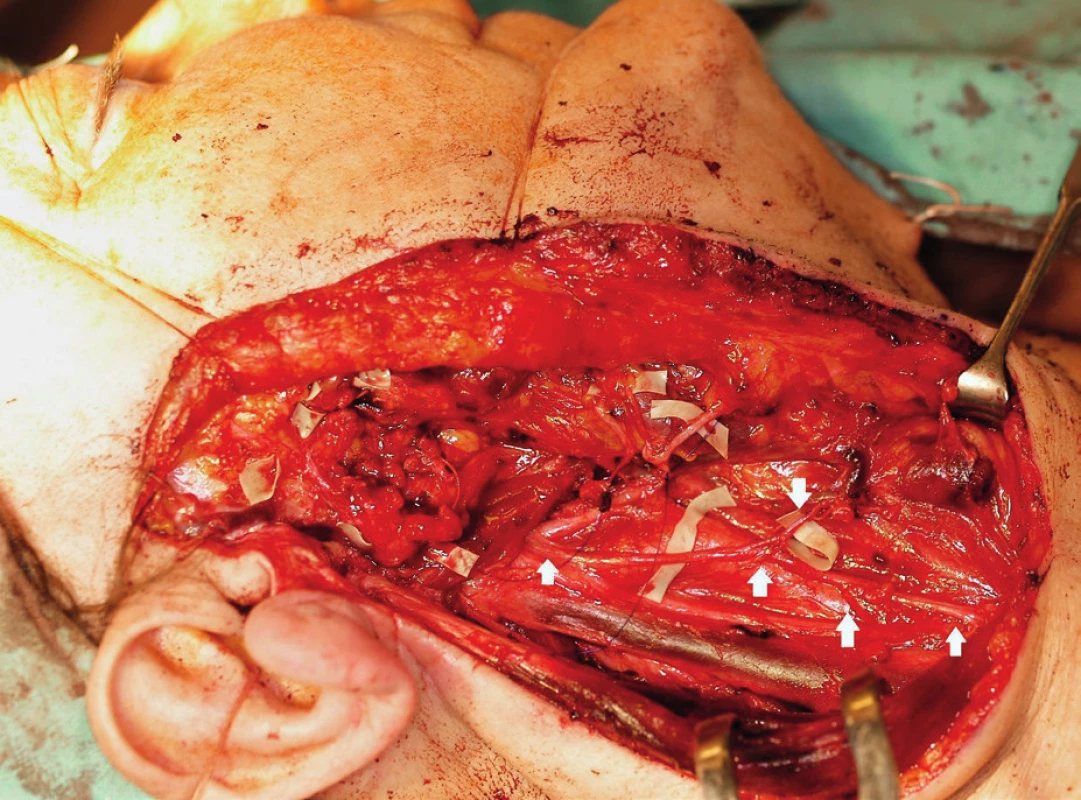
3. Intraoperative photo and anastomosis layout (anastomosis with marginal branch (Ma), and upper and lower buccal branches (B1a, B2a)). 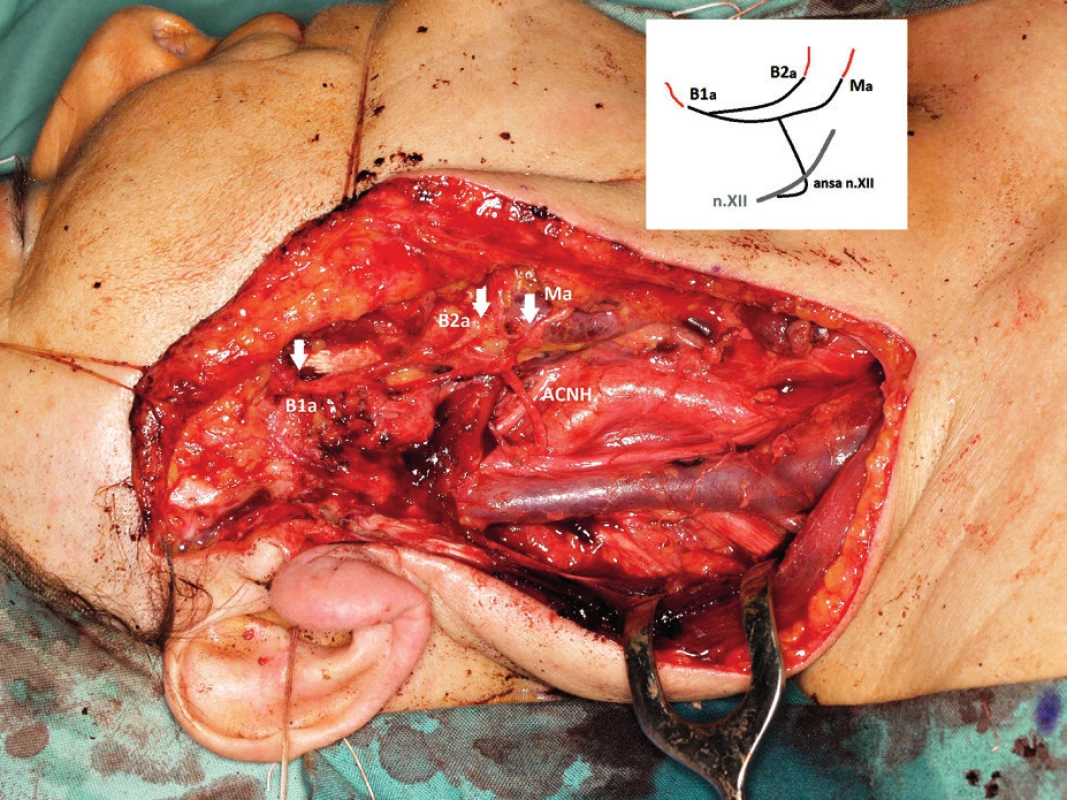
The function of the right facial nerve was monitored clinically and by electromyography in intervals of 1, 3, 6 and 12 months after the operation. Physiotherapy sessions were also organised. On later follow-ups in 6 and 12 months’ time the decrease of abnormal neuromuscular activity and stable signs of re-innervation were confirmed. The final grade of facial nerve paralysis a year after the operation was III-IV according to the House-Brackmann scale (fig. 4, 5).
Fig. 4, 5 Postoperative result – 6 months after operation. 
DISCUSSION
Large salivary gland carcinomas are a relatively rare group of tumours that represent just 2% of head and neck cancer (1). The WHO classification defines 24 types of tumours of which mucoepidermoid, acinar and adenoid cystic carcinoma have the highest prevalence rate (2).
Adenoid cystic carcinoma (ACC) represents approximately 10-15% of salivary gland malignancies. It is a slow-growing tumour for which local invasiveness and tendency for hematogenous metastasis is very typical. The aggressiveness of the tumour is due to an incomplete tumour capsule, responsible for its frequent invasion into the surrounding tissues and the high probability of perineural invasion (3). Metastases to cervical lymph nodes are rare and occur only in 8-13% of patients. In contrast, hematogenous metastases to the lungs, abdominal parenchymatous organs and bones reach 50%.
In the case of resectable tumours, radical resection, together with surgical treatment of the regional lymphatic system is indicated. The use of adjuvant radiotherapy in parotid gland ACC remains controversial. Patients should be irradiated in cases where a very close proximity or positive surgical margins are shown on histology. This also applies to cases with cervical node metastasis.
If the tumour proximity or invasion requires a facial nerve resection a reconstruction is advisable during the same operation (4). The negative surgical margins are an essential prerequisite of such a reconstruction, which has to be verified by a intra-operative frozen section histology from the nerve stumps (5).
Three main surgical techniques can be used to restore the facial nerve function after radical resection of parotid gland. 1. a nerve graft interposition, 2. a nerve transposition from which the hypoglosso-facial anastomosis is the most used. 3. the combination of these two approaches can be used which applies especially to the case of cross-facial nerve grafts of jump hypoglosso-facial nerve grafts. The cross-facial nerve grafts are not, however, used for primary facial nerve reconstruction.
The first option for reconstruction is the use of interposed nerve grafts which are harvested either from locally available sensory nerves, such as the great auricular nerve or other parts of the cervical plexus, or from distant areas such as the sural nerve. The disadvantage of this technique is the necessity of a double suture, which markedly reduces functional results of subsequent re-inervation (6). In the case of total radical parotidectomy, this technique is suboptimal also due to the fact that patients often undergo adjuvant radiotherapy which reduces blood supply and brings oxidative stress to the graft. These circumstances make the functional results of the reconstruction even worse.
The second option is the use of a transpositional anastomosis, where the donor nerve is sutured to the recipient peripheral stumps of the facial nerve. The most used donor nerve for this technique is the hypoglossal nerve for a hypogloso-facial anastomosis (HFA). This technique has better chances for a positive result (facial nerve paralysis improves to grade IV according to House-Brackmann scale or better) in approximately 70% of cases. Transsection of the hypoglossal nerve is however associated with a serious neurological deficit in terms of paralysis and atrophy of the half of the tongue, causing symptoms of swallowing difficulties and speech disorders. Moreover, this technique is also associated with a high percentage of undesirable facial synkinesis (7).
To reduce the above mentioned undesirable treatment outcomes, new modifications of this technique have been developed which can lead to a decrease of morbidity at the donor site. They are based upon partial transsection and longitudinal division of a segment of the hypoglossal nerve and its transposition and suture to the peripheral stumps of the facial nerve, so that a part of the hypoglossal nerve is preserved for tongue innervation („split n.XII - n.VII transfer“) and also use of an interposed nerve graft from hypoglossal to facial nerve “side to end HFA” (n.XII - n.VII jump graft“). These techniques of course can reduce but cannot fully eliminate the unwanted symptoms at the donor site (8).
In our case, the cervical ansa of the hypoglossal nerve was utilized to reconstruct and restore the facial nerve function (cervical ansa hypoglosso-facial anastomosis CA-HFA). The ansa is formed by branches originating from the spinal segments C1-C3 of the cervical plexus. The fibers from the ventral branch C1 are added to the fibers of n. XII. In the carotid triangle they get separated again from n. XII and descend distally forming the common neural loop with the fibbers of the ventral branch segments C2 and C3 called the ansa cervicalis profunda. Three variable branches innervating the omohyoid, sternohyoid and sternothyreoid muscles are derived from the ansa which do not originate from n. XII. Therefore, the greatest advantage of this technique is minimal morbidity at the donor site, since the cervical ansa innervates only the strap muscles which de-innervation does not cause a significant functional deficit.
Only a few reports about this technique are available in the literature (9). Despite the limited literature resources, the CA-HFA is reported to completely eliminate the undesirable symptoms of HFA. The limited use of this technique might be due to the fact that the cervical ansa usually has a very small calibre, with often insufficient numbers of nerve fibres and, therefore, it is also reported to be inadequate for use for restoration of facial nerve function and, consequently, unlikely to achieve a good postoperative result. However, our case showed a remarkable resilience of the facial nerve function even after the radiotherapy.
CONCLUSION
ACNH grafting of the facial nerve, represents a valuable alternative method for restoration of the facial nerve function, following ablative surgery of the parotid gland. The calibre of ACNH may, however, limit its practical use in some cases. Under the good anatomical circumstances this technique should be prioritized, due to less morbidity at the donor site.
Adresa ke korespondenci:
MUDr. Břetislav Gál, Ph.D.
Klinika ORL a chirurgie hlavy a krku
FN U sv. Anny
Pekařská 53 656 91 Brno
e-mail: b.gal@fnusa.cz
Labels
Audiology Paediatric ENT ENT (Otorhinolaryngology)
Article was published inOtorhinolaryngology and Phoniatrics

2018 Issue 3-
All articles in this issue
- Endoscopic Resection of Juvenile Nasopharyngeal Angiofibroma
- Role of Audiological Methods in Diagnostics of Lesions in the Pontocerebellar Angle
- Spontaneous Sublingual Haematoma as a Manifestation of an Acquired Haemophilia
- Silent Sinus Syndrome
- ENT Manifestation of Mucopolysaccharidoses
- The Survey of Implants for Bone-Conducted Hearing and Active Middle Ear Implants
- Facial Nerve Reconstruction Following Ablative Parotid Surgery - The Ansa Cervicalis Hypoglossal-Facial Anastomosis: A Case Report and Review of Literature
- Otorhinolaryngology and Phoniatrics
- Journal archive
- Current issue
- Online only
- About the journal
Most read in this issue- The Survey of Implants for Bone-Conducted Hearing and Active Middle Ear Implants
- Spontaneous Sublingual Haematoma as a Manifestation of an Acquired Haemophilia
- Silent Sinus Syndrome
- Role of Audiological Methods in Diagnostics of Lesions in the Pontocerebellar Angle
Login#ADS_BOTTOM_SCRIPTS#Forgotten passwordEnter the email address that you registered with. We will send you instructions on how to set a new password.
- Career

